Items filtered by date: October 2018
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
There Are Several Causes of Heel Pain
 Many people experience heel pain at some point in their lives. Research has shown the most common type of this uncomfortable condition is referred to as plantar fasciitis. This affects the band of tissue known as the plantar fascia, which connects the heel to the toes. Inflammation may gradually develop as a result of high or low arches or if an injury to the foot has occurred. Bursitis in the heel is another form of foot pain, and may be a result of wearing shoes that do not fit correctly. This type of inflammation originates in the fluid-filled bursa, which is located at the back of the heel. Additionally, a condition known as heel bumps typically affect teenagers. This may be a result of wearing shoes that cause friction on the underdeveloped heel bone. If the Achilles tendon should endure an injury, severe pain is generally felt in the back of the heel and may gravitate to the back of the calf. If you are experiencing heel pain, it’s suggested to speak to a podiatrist who can determine the cause and begin proper treatment as quickly as possible.
Many people experience heel pain at some point in their lives. Research has shown the most common type of this uncomfortable condition is referred to as plantar fasciitis. This affects the band of tissue known as the plantar fascia, which connects the heel to the toes. Inflammation may gradually develop as a result of high or low arches or if an injury to the foot has occurred. Bursitis in the heel is another form of foot pain, and may be a result of wearing shoes that do not fit correctly. This type of inflammation originates in the fluid-filled bursa, which is located at the back of the heel. Additionally, a condition known as heel bumps typically affect teenagers. This may be a result of wearing shoes that cause friction on the underdeveloped heel bone. If the Achilles tendon should endure an injury, severe pain is generally felt in the back of the heel and may gravitate to the back of the calf. If you are experiencing heel pain, it’s suggested to speak to a podiatrist who can determine the cause and begin proper treatment as quickly as possible.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of The Podiatry Center, PC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Millburn, NJ. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Heel PainThere Are Several Causes of Heel Pain
 Many people experience heel pain at some point in their lives. Research has shown the most common type of this uncomfortable condition is referred to as plantar fasciitis. This affects the band of tissue known as the plantar fascia, which connects the heel to the toes. Inflammation may gradually develop as a result of high or low arches or if an injury to the foot has occurred. Bursitis in the heel is another form of foot pain, and may be a result of wearing shoes that do not fit correctly. This type of inflammation originates in the fluid-filled bursa, which is located at the back of the heel. Additionally, a condition known as heel bumps typically affect teenagers. This may be a result of wearing shoes that cause friction on the underdeveloped heel bone. If the Achilles tendon should endure an injury, severe pain is generally felt in the back of the heel and may gravitate to the back of the calf. If you are experiencing heel pain, it’s suggested to speak to a podiatrist who can determine the cause and begin proper treatment as quickly as possible.
Many people experience heel pain at some point in their lives. Research has shown the most common type of this uncomfortable condition is referred to as plantar fasciitis. This affects the band of tissue known as the plantar fascia, which connects the heel to the toes. Inflammation may gradually develop as a result of high or low arches or if an injury to the foot has occurred. Bursitis in the heel is another form of foot pain, and may be a result of wearing shoes that do not fit correctly. This type of inflammation originates in the fluid-filled bursa, which is located at the back of the heel. Additionally, a condition known as heel bumps typically affect teenagers. This may be a result of wearing shoes that cause friction on the underdeveloped heel bone. If the Achilles tendon should endure an injury, severe pain is generally felt in the back of the heel and may gravitate to the back of the calf. If you are experiencing heel pain, it’s suggested to speak to a podiatrist who can determine the cause and begin proper treatment as quickly as possible.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of The Podiatry Center, PC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Millburn, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes Symptoms and Treatment for Poor Circulation in the Feet
The purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
Causes Symptoms and Treatment for Poor Circulation in the Feet
The purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
Symptoms of Poor Circulation
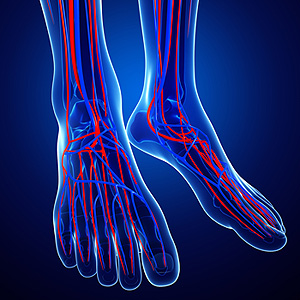 If you have poor circulation, it may be indicative of other conditions that may be present in the body. A proper diagnosis is necessary in determining if you may possibly have peripheral artery disease, blood clots, or a heart condition. There are common symptoms that may be associated with this ailment including experiencing a tingling sensation in the feet, being tired the majority of the time, or water weight gain, which may also be referred to as edema. Additionally, some patients may experience muscle cramps, pain in the feet, or a general feeling of weakness. Research has shown that poor habits regarding your health may play a significant role. These may include a lack of exercise, or an excess amount of smoking or alcohol consumption. If you are experiencing any of these symptoms, it's important to speak with a podiatrist as quickly as possible so the right course of treatment can begin.
If you have poor circulation, it may be indicative of other conditions that may be present in the body. A proper diagnosis is necessary in determining if you may possibly have peripheral artery disease, blood clots, or a heart condition. There are common symptoms that may be associated with this ailment including experiencing a tingling sensation in the feet, being tired the majority of the time, or water weight gain, which may also be referred to as edema. Additionally, some patients may experience muscle cramps, pain in the feet, or a general feeling of weakness. Research has shown that poor habits regarding your health may play a significant role. These may include a lack of exercise, or an excess amount of smoking or alcohol consumption. If you are experiencing any of these symptoms, it's important to speak with a podiatrist as quickly as possible so the right course of treatment can begin.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact one of our podiatrists of The Podiatry Center, PC. Our doctors will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
- Numbness
- Tingling
- Throbbing or stinging pain in limbs
- Pain
- Muscle Cramps
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our office located in Millburn, NJ. We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Causes Symptoms and Treatment for Poor Circulation in the FeetSymptoms of Poor Circulation
 If you have poor circulation, it may be indicative of other conditions that may be present in the body. A proper diagnosis is necessary in determining if you may possibly have peripheral artery disease, blood clots, or a heart condition. There are common symptoms that may be associated with this ailment including experiencing a tingling sensation in the feet, being tired the majority of the time, or water weight gain, which may also be referred to as edema. Additionally, some patients may experience muscle cramps, pain in the feet, or a general feeling of weakness. Research has shown that poor habits regarding your health may play a significant role. These may include a lack of exercise, or an excess amount of smoking or alcohol consumption. If you are experiencing any of these symptoms, it's important to speak with a podiatrist as quickly as possible so the right course of treatment can begin.
If you have poor circulation, it may be indicative of other conditions that may be present in the body. A proper diagnosis is necessary in determining if you may possibly have peripheral artery disease, blood clots, or a heart condition. There are common symptoms that may be associated with this ailment including experiencing a tingling sensation in the feet, being tired the majority of the time, or water weight gain, which may also be referred to as edema. Additionally, some patients may experience muscle cramps, pain in the feet, or a general feeling of weakness. Research has shown that poor habits regarding your health may play a significant role. These may include a lack of exercise, or an excess amount of smoking or alcohol consumption. If you are experiencing any of these symptoms, it's important to speak with a podiatrist as quickly as possible so the right course of treatment can begin.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact one of our podiatrists of The Podiatry Center, PC. Our doctors will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
- Numbness
- Tingling
- Throbbing or stinging pain in limbs
- Pain
- Muscle Cramps
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our office located in Millburn, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Causes Symptoms and Treatment for Poor Circulation in the FeetHow to Deal with Athlete's Foot
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.
How to Deal with Athlete's Foot
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.
